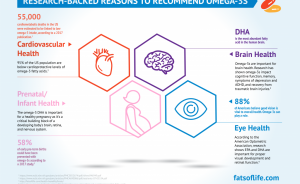
90% of people worldwide are below cardioprotective levels of omega-3s.
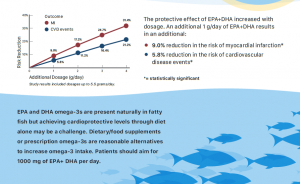
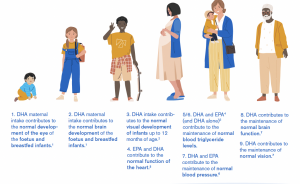
EPA and DHA omega-3s have solid research for a variety of heart health outcomes. EPA and DHA have been shown to have a statistically significant reduction in systolic and diastolic blood pressure, a risk factor for coronary heart disease. In addition, an increased intake of EPA and DHA omega-3s has been shown to significantly reduce serum triglycerides. Additionally, there is considerable evidence for the role of omega-3s in reducing heart rate as well as heart rate variability.
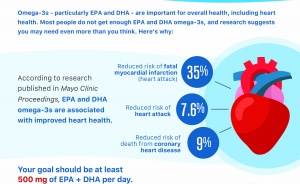
Further, research supports the importance of EPA and DHA for a variety of cardiovascular outcomes, including reducing the risk of coronary heart disease, myocardial infarction and cardiac death. Omega-3s also support healthy blood vessels by decreasing arterial stiffness and increasing endothelial function.
Patients with cardiovascular risk factors may experience more effect from increased EPA and DHA intake. Research is ongoing to understand the role of omega-3s and the risk, prevention, and/or treatment of atrial fibrillation.
See resources below, or ask us about the many more reasons to recommend omega-3s for your patient's heart.